Connect With Us
Blog
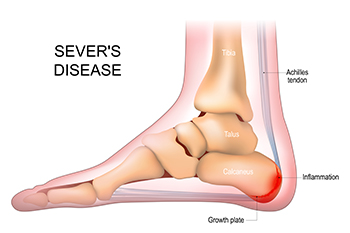
Sever's disease, despite its name, is not an illness, but a common heel bone disorder that affects children during their growth spurts. Also known as calcaneal apophysitis, this condition occurs when the heel's growth plate experiences inflammation due to repetitive stress and tension. Typically afflicting children aged 8 to 14, Sever's disease emerges as the bones grow faster than the tendons, leading to strain on the heel's growth plate. Young athletes engaged in high-impact sports, such as soccer, basketball, and gymnastics, are particularly susceptible. The symptoms can include heel pain, swelling, and discomfort, which can be worse during physical activities. Recognizing Sever's disease is important, as prompt intervention can alleviate symptoms and prevent long-term complications. If your child has heel pain, and frequently participates in sporting activities, it is suggested that you consult a podiatrist who can accurately diagnose and treat this condition.
Sever's disease often occurs in children and teens. If your child is experiencing foot or ankle pain, see Dr. Michael D. Garvin from Florida. Our doctor can treat your child’s foot and ankle needs.
Sever’s Disease
Sever’s disease is also known as calcaneal apophysitis, which is a medical condition that causes heel pain I none or both feet. The disease is known to affect children between the ages of 8 and 14.
Sever’s disease occurs when part of the child’s heel known as the growth plate (calcaneal epiphysis) is attached to the Achilles tendon. This area can suffer injury when the muscles and tendons of the growing foot do not keep pace with bone growth. Therefore, the constant pain which one experiences at the back of the heel will make the child unable to put any weight on the heel. The child is then forced to walk on their toes.
Symptoms
Acute pain – Pain associated with Sever’s disease is usually felt in the heel when the child engages in physical activity such as walking, jumping and or running.
Highly active – Children who are very active are among the most susceptible in experiencing Sever’s disease, because of the stress and tension placed on their feet.
If you have any questions, please feel free to contact our offices located in Port St. Lucie, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle injuries.
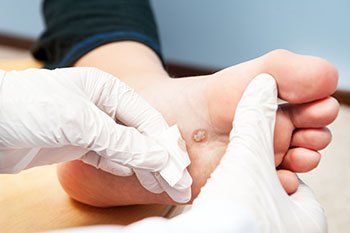
Plantar warts, caused by the human papillomavirus, HPV, can develop in anyone, but certain factors may heighten vulnerability. Individuals with weakened immune systems are at an increased risk, as the body's defense mechanisms struggle to combat the viral invader. The symptoms of plantar warts often include small, fleshy growths on the soles of the feet, accompanied by tenderness or pain while walking. Children and teenagers, with developing immune systems, are particularly susceptible to these uncomfortable growths. Prolonged exposure to moist environments, such as communal showers or swimming pools, also escalates the risk. Additionally, those who frequently walk barefoot in public spaces may find themselves more prone to contracting the virus. If you have developed a plantar wart, it is strongly suggested that you visit a podiatrist who can offer effective treatment options and prevention tips.
Plantar warts can be very uncomfortable. If you need your feet checked, contact Dr. Michael D. Garvin from Florida. Our doctor will assist you with all of your foot and ankle needs.
About Plantar Warts
Plantar warts are the result of HPV, or human papillomavirus, getting into open wounds on the feet. They are mostly found on the heels or balls of the feet.
While plantar warts are generally harmless, those experiencing excessive pain or those suffering from diabetes or a compromised immune system require immediate medical care. Plantar warts are easily diagnosed, usually through scraping off a bit of rough skin or by getting a biopsy.
Symptoms
- Lesions on the bottom of your feet, usually rough and grainy
- Hard or thick callused spots
- Wart seeds, which are small clotted blood vessels that look like little black spots
- Pain, discomfort, or tenderness of your feet when walking or standing
Treatment
- Freezing
- Electric tool removal
- Laser Treatment
- Topical Creams (prescription only)
- Over-the-counter medications
To help prevent developing plantar warts, avoid walking barefoot over abrasive surfaces that can cause cuts or wounds for HPV to get into. Avoiding direct contact with other warts, as well as not picking or rubbing existing warts, can help prevent the further spread of plantar warts. However, if you think you have developed plantar warts, speak to your podiatrist. He or she can diagnose the warts on your feet and recommend the appropriate treatment options.
If you have any questions please feel free to contact our offices located in Port St. Lucie, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
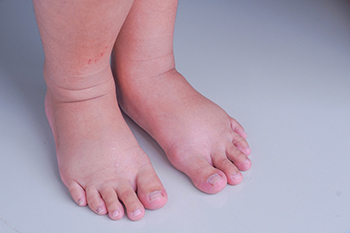
Swollen feet, or edema, can disrupt daily life. This condition often has a spectrum of common causes that individuals should be attuned to for timely intervention and relief. Prolonged periods of standing or sitting, especially in positions that impede healthy blood circulation, can lead to fluid retention, resulting in swollen feet. Another frequent contributor is the choice of footwear, with ill-fitting shoes or high heels imposing pressure that hinders proper blood flow. Injuries, such as sprains or fractures, can trigger inflammation and swelling in the affected area. Underlying medical conditions, including venous insufficiency, arthritis, or heart failure, may manifest in swollen feet. Hormonal changes during pregnancy often result in fluid retention, causing noticeable swelling in the feet and ankles. Lifestyle factors, like a diet high in sodium, can exacerbate fluid retention. Swollen feet can be uncomfortable, and if you have this condition, it is suggested that you visit a podiatrist who can accurately determine the cause, and offer appropriate treatment tips.
Swollen feet can be a sign of an underlying condition. If you have any concerns, contact Dr. Michael D. Garvin of Florida. Our doctor can provide the care you need to keep you pain-free and on your feet.
Swollen feet are a common ailment among pregnant women and people who stand or sit for extended periods. Aging may increase the possibility of swollen feet and patients who are obese often notice when their feet are swelling too. There may be medical reasons why swollen feet occur:
- Phlebitis - A condition that causes the veins to become inflamed and can also cause leg pain.
- Liver disease - This may lead to low blood levels of albumin which is a protein. This can cause fluid in the blood to pass into the tissues and several areas of the body can become swollen.
- Heart failure - When the heart doesn’t pump properly the blood that is normally pumped back to the heart can pool in the veins of the legs causing swollen feet.
- Kidney disease - One of the main functions of the kidneys is releasing excess fluid in the body. This type of condition can make it difficult for the kidneys to function properly, and as a result the feet may become swollen.
- Deep-vein thrombosis (DVT)- This is a serious condition where blood clots form in the veins of the legs. They can block the return of blood from the legs to the heart which may cause the feet to swell. It is important to be treated by a podiatrist if this condition is present.
Swollen feet can also be caused by bone and tendon conditions, including fractures, arthritis, and tendinitis. Additionally, there may be skin and toenail conditions and an infection may cause the feet to swell. Patients who take medicine to treat high blood pressure may be prone to getting swollen feet.
Many patients elevate their feet to help relieve the swelling and this is generally a temporary remedy. When a podiatrist is consulted the reason behind the swelling can be uncovered and subsequently treated.
If you have any questions please feel free to contact our offices located in Port St. Lucie, FL . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
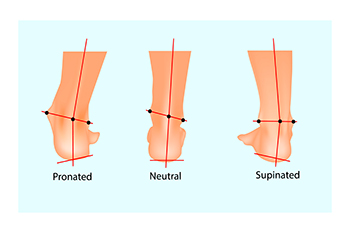
Overpronation, the inward rolling of the foot during the gait cycle, can pose challenges for runners, potentially leading to various injuries. While some pronation is natural and necessary, excessive overpronation may result in plantar fasciitis and other conditions. The delicate balance between foot mobility and stability is important for runners who repeatedly land on one leg. Ankle stability plays a pivotal role in healthy running, and choosing the right running shoes is a key factor. To determine your pronation type, stand on one foot in front of a mirror and observe any wobbling or medial arch collapse. For those who overpronate, selecting shoes with medial arch support and a wider heel can enhance stability during runs. Addressing overpronation involves strengthening weakened muscles. Exercises such as squats, calf raises, lunges, and single-leg deadlifts contribute to foot and ankle strength. Specific drills like heel walks and toe walks target foot stabilizers and may reduce the risk of overpronation-related injuries. Understand your pronation type and incorporate targeted exercises to mitigate injury risks. For a full gait analysis and pronation assessment, it is suggested that you schedule an appointment with a podiatrist.
If you have any concerns about your feet, contact Dr. Michael D. Garvin from Florida. Our doctor can provide the care you need to keep you pain-free and on your feet.
Biomechanics in Podiatry
Podiatric biomechanics is a particular sector of specialty podiatry with licensed practitioners who are trained to diagnose and treat conditions affecting the foot, ankle and lower leg. Biomechanics deals with the forces that act against the body, causing an interference with the biological structures. It focuses on the movement of the ankle, the foot and the forces that interact with them.
A History of Biomechanics
- Biomechanics dates back to the BC era in Egypt where evidence of professional foot care has been recorded.
- In 1974, biomechanics gained a higher profile from the studies of Merton Root, who claimed that by changing or controlling the forces between the ankle and the foot, corrections or conditions could be implemented to gain strength and coordination in the area.
Modern technological improvements are based on past theories and therapeutic processes that provide a better understanding of podiatric concepts for biomechanics. Computers can provide accurate information about the forces and patterns of the feet and lower legs.
Understanding biomechanics of the feet can help improve and eliminate pain, stopping further stress to the foot.
If you have any questions please feel free to contact our offices located in Port St. Lucie, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Blog Archives
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
- December 2018
- November 2018
- October 2018
- September 2018
- August 2018
- July 2018
- June 2018
- May 2018
- April 2018
- March 2018
- February 2018
- January 2018
- December 2017
- November 2017
- October 2017
- September 2017
- August 2017
- July 2017
- June 2017
- May 2017
- April 2017
- March 2017
- February 2017
- January 2017
- December 2016
- November 2016
- October 2016
- September 2016
- August 2016
