Connect With Us
Featured Articles
Items filtered by date: January 2021
Dealing with Stress Fractures of the Foot and Ankle
Stress fractures are small breaks in the bone that are caused by repetitive stress. They typically occur due to overuse, forcing the bones of the foot or ankle to continually absorb the full impact of each step taken. Stress fractures can also be caused by abnormal foot structure, osteoporosis, bone deformities, or wearing improper footwear during exercise.
Stress fractures are common for individuals whose daily activities cause high levels of impact on their feet and ankles. Those who run, play tennis or basketball, or practice gymnastics tend to experience these fractures more frequently. Anyone is susceptible to this problem, though. Individuals who are normally sedentary and suddenly begin an intense, high impact workout may sustain stress fractures. This is because their muscles are not yet strong enough to handle and cushion the intensity of their activity. Osteoporosis may also cause someone to get stress fractures, because the disease weakens an afflicted person's bones and makes it easier for them to break down.
Pain from stress fractures typically occurs in the general area of the fracture. Pain can also manifest as “pinpoint pain” or pain that is felt when the site of the injury is touched, and can be accompanied by swelling. It may occur during or after activity, and it may disappear while resting and return when standing or moving. Engaging in any kind of activity, high impact or otherwise, will aggravate the pain. If the intensity of the activity increases before the stress fracture has properly healed, it can cause a full fracture.
Treatment can vary depending on the individual and the degree of injury. The primary way to treat a stress fracture is to rest the hurt foot. Some fractures will heal quickly with only a little bit of rest, while others may require a long rest period and the use of crutches, immobilization, or physical therapy. Under certain circumstances, surgery may be required to install support pins around the fracture to assist in healing.
If you are undergoing a new exercise regimen in running or some other kind of high impact activity, set incremental goals on a weekly basis so you can build up muscle strength. Make sure to wear supportive shoes to better protect you feet.
If you begin to experience any symptoms of stress fractures, you should stop exercising and rest. If the symptoms persist, consult with your podiatrist. Remembering these tips can help you prevent stress fractures to your foot and ankle, and allow you to continue living normally.
Dealing with Stress Fractures of the Foot and Ankle
Stress fractures are small breaks in the bone that are caused by repetitive stress. They typically occur due to overuse, forcing the bones of the foot or ankle to continually absorb the full impact of each step taken. Stress fractures can also be caused by abnormal foot structure, osteoporosis, bone deformities, or wearing improper footwear during exercise.
Stress fractures are common for individuals whose daily activities cause high levels of impact on their feet and ankles. Those who run, play tennis or basketball, or practice gymnastics tend to experience these fractures more frequently. Anyone is susceptible to this problem, though. Individuals who are normally sedentary and suddenly begin an intense, high impact workout may sustain stress fractures. This is because their muscles are not yet strong enough to handle and cushion the intensity of their activity. Osteoporosis may also cause someone to get stress fractures, because the disease weakens an afflicted person's bones and makes it easier for them to break down.
Pain from stress fractures typically occurs in the general area of the fracture. Pain can also manifest as “pinpoint pain” or pain that is felt when the site of the injury is touched, and can be accompanied by swelling. It may occur during or after activity, and it may disappear while resting and return when standing or moving. Engaging in any kind of activity, high impact or otherwise, will aggravate the pain. If the intensity of the activity increases before the stress fracture has properly healed, it can cause a full fracture.
Treatment can vary depending on the individual and the degree of injury. The primary way to treat a stress fracture is to rest the hurt foot. Some fractures will heal quickly with only a little bit of rest, while others may require a long rest period and the use of crutches, immobilization, or physical therapy. Under certain circumstances, surgery may be required to install support pins around the fracture to assist in healing.
If you are undergoing a new exercise regimen in running or some other kind of high impact activity, set incremental goals on a weekly basis so you can build up muscle strength. Make sure to wear supportive shoes to better protect you feet.
If you begin to experience any symptoms of stress fractures, you should stop exercising and rest. If the symptoms persist, consult with your podiatrist. Remembering these tips can help you prevent stress fractures to your foot and ankle, and allow you to continue living normally.
Diagnosing and Healing Stress Fractures
 People who enjoy running and jogging often fear enduring a stress fracture. This is a hairline fracture, a tiny crack in the bone that can gradually develop as a result of repeated force against the bone. Common symptoms of a stress fracture in the foot can include dull pain, mild swelling, and weakness. These symptoms are often ignored, and can become worse if proper healing measures are not implemented. Dedicated runners will often run through the pain, and it may become unbearable to put weight on the affected foot. Stress fractures are generally diagnosed by having an X-ray taken. Once a stress fracture is detected, it is often suggested that you stop running for several weeks. If you have pain in your foot and think that it may be a stress fracture, please consult with a podiatrist who can offer you effective treatment options.
People who enjoy running and jogging often fear enduring a stress fracture. This is a hairline fracture, a tiny crack in the bone that can gradually develop as a result of repeated force against the bone. Common symptoms of a stress fracture in the foot can include dull pain, mild swelling, and weakness. These symptoms are often ignored, and can become worse if proper healing measures are not implemented. Dedicated runners will often run through the pain, and it may become unbearable to put weight on the affected foot. Stress fractures are generally diagnosed by having an X-ray taken. Once a stress fracture is detected, it is often suggested that you stop running for several weeks. If you have pain in your foot and think that it may be a stress fracture, please consult with a podiatrist who can offer you effective treatment options.
Activities where too much pressure is put on the feet can cause stress fractures. To learn more, contact Dr. Michael D. Garvin from Florida. Our doctor can provide the care you need to keep your pain free and on your feet.
Dealing with Stress Fractures of the Foot and Ankle
Stress fractures occur in the foot and ankle when muscles in these areas weaken from too much or too little use. The feet and ankles then lose support when walking or running from the impact of the ground. Since there is no protection, the bones receive the full impact of each step. Stress on the feet can cause cracks to form in the bones, thus creating stress fractures.
What Are Stress Fractures?
Stress fractures occur frequently in individuals whose daily activities cause great impact on the feet and ankles. Stress factors are most common among:
- Runners
- People affected with Osteoporosis
- Tennis or basketball players
- Gymnasts
- High impact workouts
Symptoms
Pain from the fractures occur in the area of the fractures and can be constant or intermittent. It will often cause sharp or dull pain with swelling and tenderness. Engaging in any kind of activity which involves high impact will aggravate pain.
If you have any questions please feel free to contact our offices located in Port St. Lucie, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Read more about Dealing with Stress Fractures of the Foot and AnkleDiagnosing and Healing Stress Fractures
 People who enjoy running and jogging often fear enduring a stress fracture. This is a hairline fracture, a tiny crack in the bone that can gradually develop as a result of repeated force against the bone. Common symptoms of a stress fracture in the foot can include dull pain, mild swelling, and weakness. These symptoms are often ignored, and can become worse if proper healing measures are not implemented. Dedicated runners will often run through the pain, and it may become unbearable to put weight on the affected foot. Stress fractures are generally diagnosed by having an X-ray taken. Once a stress fracture is detected, it is often suggested that you stop running for several weeks. If you have pain in your foot and think that it may be a stress fracture, please consult with a podiatrist who can offer you effective treatment options.
People who enjoy running and jogging often fear enduring a stress fracture. This is a hairline fracture, a tiny crack in the bone that can gradually develop as a result of repeated force against the bone. Common symptoms of a stress fracture in the foot can include dull pain, mild swelling, and weakness. These symptoms are often ignored, and can become worse if proper healing measures are not implemented. Dedicated runners will often run through the pain, and it may become unbearable to put weight on the affected foot. Stress fractures are generally diagnosed by having an X-ray taken. Once a stress fracture is detected, it is often suggested that you stop running for several weeks. If you have pain in your foot and think that it may be a stress fracture, please consult with a podiatrist who can offer you effective treatment options.
Activities where too much pressure is put on the feet can cause stress fractures. To learn more, contact Dr. Michael D. Garvin from Florida. Our doctor can provide the care you need to keep your pain free and on your feet.
Dealing with Stress Fractures of the Foot and Ankle
Stress fractures occur in the foot and ankle when muscles in these areas weaken from too much or too little use. The feet and ankles then lose support when walking or running from the impact of the ground. Since there is no protection, the bones receive the full impact of each step. Stress on the feet can cause cracks to form in the bones, thus creating stress fractures.
What Are Stress Fractures?
Stress fractures occur frequently in individuals whose daily activities cause great impact on the feet and ankles. Stress factors are most common among:
- Runners
- People affected with Osteoporosis
- Tennis or basketball players
- Gymnasts
- High impact workouts
Symptoms
Pain from the fractures occur in the area of the fractures and can be constant or intermittent. It will often cause sharp or dull pain with swelling and tenderness. Engaging in any kind of activity which involves high impact will aggravate pain.
If you have any questions please feel free to contact our offices located in Port St. Lucie, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
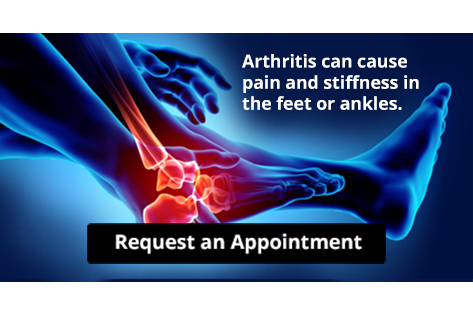
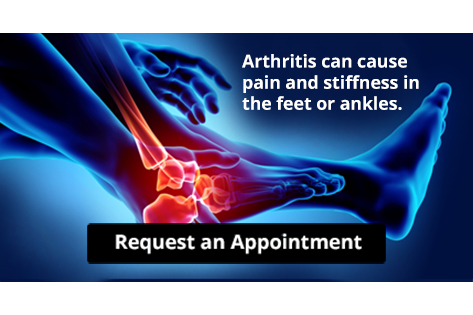
Arthritis Can Cause Pain in the Feet and Ankles
Arthritis Can Cause Pain in the Feet and Ankles
Sever's Disease
Sever's disease, also known as calcaneal apophysitis, is a medical condition that causes heel pain in children’s feet while they’re growing. Sever's disease occurs most commonly in boys and girls between the ages of 8 and 14.
Sever's disease occurs when the child’s growth plate, or the calcaneal epiphysis, an area attached to the Achilles tendon, is injured or when the muscles and tendons of the growing foot do not keep pace with bone growth. The result is constant pain experienced at the back of the heel and the inability to put any weight on the heel. This forces the child to bear weight on their toes while walking. When a toe gait develops, the child must change the way they walk to avoid placing weight on the painful heel. If this is not properly addressed, this can lead to further developmental problems.
The most common symptom of Sever's disease is acute pain felt in the heel when a child engages in physical activity such as walking, jumping or running. Children who are active athletes are among the group most susceptible to experiencing Sever's disease. This is due to the extreme stress and tension placed on their growing feet. The rolling movement of the foot during walking or running and obesity are both additional conditions linked to causing Sever's disease.
The first step in treating Sever's disease is to rest the foot and leg and avoid physical activity. Over the counter pain-relieving and anti-inflammatory medications can be helpful for reducing the amount of heel pain. A child with Sever's disease should also wear shoes that properly support the heel and the arch of the foot. Consider purchasing orthotic shoe inserts which can help support the heel and foot while it is healing. Most patients with Sever's disease symptoms report an eventual elimination of heel pain after wearing orthotic insoles that support the affected heel.
Sever's disease may affect either one heel or both. It is important for a child experiencing heel pain to be examined by a foot doctor who can apply the squeeze test. The squeeze test compresses both sides of the heel in order to determine if there is intense pain. Discourage any child diagnosed with Sever's disease from going barefoot as this can intensify the problem. Apply ice packs to the affected painful heel two or three times a day for pain relief.
Exercises that help stretch the calf muscles and hamstrings are effective at treating Sever's disease. An exercise known as foot curling has also proven to be very effective at treating Sever's disease. When foot curling, the foot is pointed away from the body, then curled toward the body to help stretch the muscles. The curling exercise should be done in sets of 10 or 20 repetitions and repeated several times throughout the day.
Treatment methods can continue for at least 2 weeks and as long as 2 months before the heel pain completely disappears. A child can continue doing daily stretching exercises for the legs and feet to prevent Sever’s disease from returning.
Who Does Sever’s Disease Affect?
 Sever’s disease primarily affects children and young teenagers. The pain that comes from this condition is felt in the heels, as its growth plate is what is often affected. Dur to the heel pain, some may experience difficulty walking. Sever’s disease can develop as a result of frequently participating in running and jumping activities. Additionally, children who have flat feet or high arches may be prone to Sever’s disease. Some of the symptoms that are associated with this ailment include increased heel pain after exercise and stiffness surrounding the affected heel. Mild relief may be found when specific stretches are performed on the heel, as well as wearing custom-made orthotics. If your child partakes in a lot of physical activity and is complaining about heel pain, please consult with a podiatrist for a proper diagnosis.
Sever’s disease primarily affects children and young teenagers. The pain that comes from this condition is felt in the heels, as its growth plate is what is often affected. Dur to the heel pain, some may experience difficulty walking. Sever’s disease can develop as a result of frequently participating in running and jumping activities. Additionally, children who have flat feet or high arches may be prone to Sever’s disease. Some of the symptoms that are associated with this ailment include increased heel pain after exercise and stiffness surrounding the affected heel. Mild relief may be found when specific stretches are performed on the heel, as well as wearing custom-made orthotics. If your child partakes in a lot of physical activity and is complaining about heel pain, please consult with a podiatrist for a proper diagnosis.
Sever's disease often occurs in children and teens. If your child is experiencing foot or ankle pain, see Dr. Michael D. Garvin from Florida. Our doctor can treat your child’s foot and ankle needs.
Sever’s Disease
Sever’s disease is also known as calcaneal apophysitis, which is a medical condition that causes heel pain I none or both feet. The disease is known to affect children between the ages of 8 and 14.
Sever’s disease occurs when part of the child’s heel known as the growth plate (calcaneal epiphysis) is attached to the Achilles tendon. This area can suffer injury when the muscles and tendons of the growing foot do not keep pace with bone growth. Therefore, the constant pain which one experiences at the back of the heel will make the child unable to put any weight on the heel. The child is then forced to walk on their toes.
Symptoms
Acute pain – Pain associated with Sever’s disease is usually felt in the heel when the child engages in physical activity such as walking, jumping and or running.
Highly active – Children who are very active are among the most susceptible in experiencing Sever’s disease, because of the stress and tension placed on their feet.
If you have any questions, please feel free to contact our offices located in Port St. Lucie, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle injuries.
Read more about Sever's DiseaseTreatments Options for Plantar Fasciitis
 Plantar fasciitis is a common foot condition in which the plantar fascia, the ligament that runs along the bottom of the foot and connects the heel bone to the toes, becomes inflamed. This leads to heel pain that tends to be at its worst in the morning and immediately after exercising. If you have plantar fasciitis, there are multiple treatment options. It is recommended that you rest the affected foot as much as possible to give it time to heal and to prevent further damage. Applying ice to the foot or taking an over-the-counter pain medication can reduce inflammation and pain. Wearing shoes that fit your feet properly and are supportive, wearing orthotic inserts in your shoes, and stretching the feet regularly can improve symptoms and decrease your likelihood of developing plantar fasciitis in the future. If you think that you are suffering from plantar fasciitis, it is recommended that you see a podiatrist for a proper diagnosis.
Plantar fasciitis is a common foot condition in which the plantar fascia, the ligament that runs along the bottom of the foot and connects the heel bone to the toes, becomes inflamed. This leads to heel pain that tends to be at its worst in the morning and immediately after exercising. If you have plantar fasciitis, there are multiple treatment options. It is recommended that you rest the affected foot as much as possible to give it time to heal and to prevent further damage. Applying ice to the foot or taking an over-the-counter pain medication can reduce inflammation and pain. Wearing shoes that fit your feet properly and are supportive, wearing orthotic inserts in your shoes, and stretching the feet regularly can improve symptoms and decrease your likelihood of developing plantar fasciitis in the future. If you think that you are suffering from plantar fasciitis, it is recommended that you see a podiatrist for a proper diagnosis.
Plantar fasciitis can be very painful and inconvenient. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Dr. Michael D. Garvin from Florida. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is the inflammation of the thick band of tissue that runs along the bottom of your foot, known as the plantar fascia, and causes mild to severe heel pain.
What Causes Plantar Fasciitis?
- Excessive running
- Non-supportive shoes
- Overpronation
- Repeated stretching and tearing of the plantar fascia
How Can It Be Treated?
- Conservative measures – anti-inflammatories, ice packs, stretching exercises, physical therapy, orthotic devices
- Shockwave therapy – sound waves are sent to the affected area to facilitate healing and are usually used for chronic cases of plantar fasciitis
- Surgery – usually only used as a last resort when all else fails. The plantar fascia can be surgically detached from the heel
While very treatable, plantar fasciitis is definitely not something that should be ignored. Especially in severe cases, speaking to your doctor right away is highly recommended to avoid complications and severe heel pain. Your podiatrist can work with you to provide the appropriate treatment options tailored to your condition.
If you have any questions please feel free to contact our offices located in Port St. Lucie, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Read more about Plantar FasciitisPlantar Fasciitis
The plantar fascia is a connective tissue in the heel that stretches across the bottom length of your foot. Plantar fasciitis occurs when the connective tissue becomes inflamed, causing heel pain and discomfort during physical activity. Although the condition is completely treatable, traditional methods can take up to a year to start becoming effective.
Plantar fasciitis is caused by a number of everyday activities, so understanding the condition is important for managing and treating it. One of the most common causes of plantar fasciitis is excessive running, especially with improper fitting or non-supportive shoes. Too much exercise can lead to the plantar fascia being overworked and overstretched, which can cause tears in the tissue. Along with improper fitting shoes, pronation, the rolling of the feet inward, is a common cause of plantar fasciitis. If not treated properly, the plantar fascia becomes overstretched and starts to tear, causing inflammation.
Despite the common causes of plantar fasciitis, there are many different treatment options. For less severe cases, conservative home remedies include taking anti-inflammatory drugs to alleviate pain, applying ice packs to the bottom of your foot and heel, slowly stretching and exercising your feet to re-strengthen the tissue, and using orthotic devices are all ways to help manage your plantar fasciitis.
For more severe cases, shockwave therapy has become a common solution for plantar fasciitis. Shockwave therapy can effectively break up the tissue on the bottom of your foot which facilitates healing and regeneration. This fights the chronic pain caused by plantar fasciitis. Even if this doesn’t work, surgery is always a final option. Surgery on the tissue itself can be done to permanently correct the issue and stop the inflammation and pain in your heels.
No matter what the case may be, consulting your podiatrist is the first and best step to recovery. Even the slightest amount of heel pain could be the first stage of plantar fasciitis. Untreated symptoms can lead to the tearing and overstretching of tissue. Because the tearing of tissue can be compounded if it remains ignored, it can evolve into a severe case. The solution is early detection and early treatment. Talk to your podiatrist about the possibilities of plantar fasciitis if you’re experiencing heel pain.
Featured Articles
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
- December 2018
- November 2018
- October 2018
- September 2018
- August 2018
- July 2018
- June 2018
- May 2018
- April 2018
- March 2018
- February 2018
- January 2018
- December 2017
- November 2017
- October 2017
- September 2017
- August 2017
- July 2017
- June 2017
- May 2017
- April 2017
- March 2017
- February 2017
- January 2017
- December 2016
- November 2016
- October 2016
- September 2016
- August 2016